TELMON-NOR
The TELMON-NOR study: Do we monitor the heart rhythm of the patients who need it most?

We investigate the extent of severe cardiac arrhythmias that occur during in-hospital telemetry monitoring and subsequent treatment. In addition, duration of monitoring is investigated. Principal investigator of the study is Nina Fålun.
Patients in need of arrhythmia monitoring are connected to a telemetry unit - a portable wireless device the size of a mobile phone. This continuously registers the heart rhythm and transmits wireless data to a central monitor station - usually located at the medical intensive care unit. Nurses, both at the intensive care units and the medical and surgical wards, are pivotal in ensuring a high quality arrhythmia monitoring.
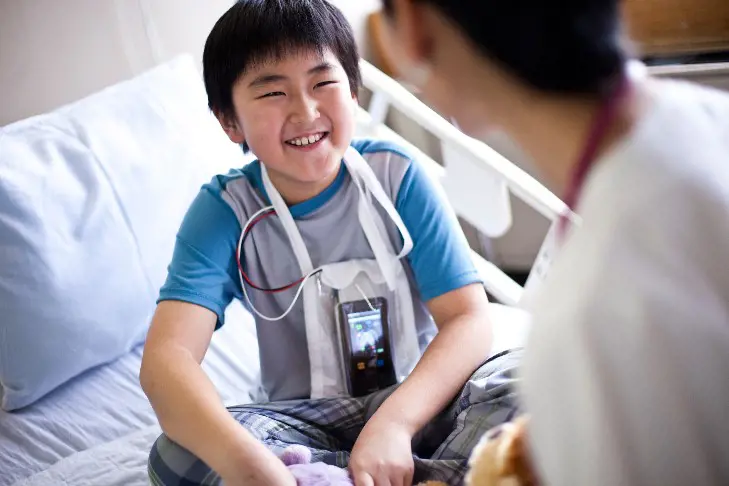
For some, telemetry monitoring are lifesaving, as potentially life-threatening arrhythmias are monitored and measures are implemented immediately if needed. For others, arrhythmias may lead to treatment with medications, cardioversion, or implantation of a pacemaker. Monitoring after various procedures and interventions such as percutaneous coronary intervention, radio frequency ablation, and cardiac surgery is also important as they can cause arrhythmias.
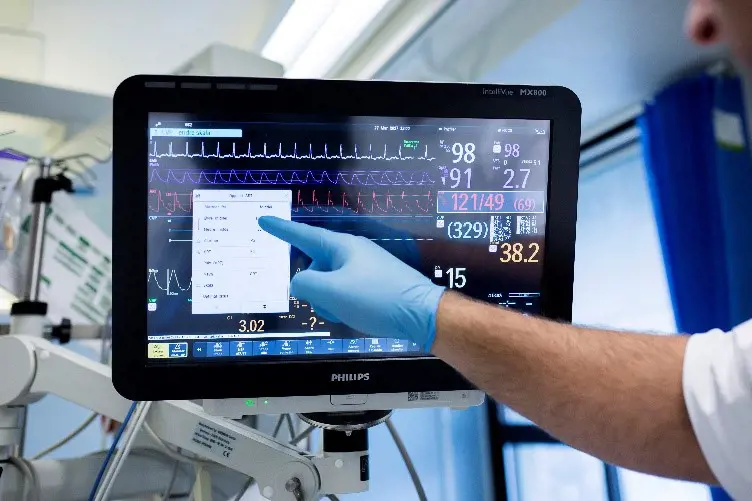
Annually, more than 6,000 patients are monitored with in-hospital telemetry at Haukeland University Hospital. The number of patients admitted to hospital with a potential for developing life-threatening arrhythmias during their hospital stay are increasing. This includes patients with confirmed myocardial infarction, patients with undiagnosed cardiovascular disease and patients with persistent and treatment-requiring arrhythmias as admission diagnosis.
In addition, patients undergoing PCI and cardiac surgery, patients with severe heart failure, and patients with various electrolyte imbalances, are monitored. Which patients benefit the most from telemetry monitoring must be adapted to new technology and new treatment options. Therefore, this will change over time. International and local guidelines for in-hospital telemetry monitoring must reflect this development.
Patient safety during the hospital stay is ensured by 24-hour continuous telemetry monitoring, by implementation of necessary measures and treatment, and by ensuring good signal quality with correct electrode placement. The development of local and national guidelines for telemetry monitoring is important to ensure that limited telemetry resources are used to benefit patients with the greatest need of arrhythmia monitoring.
TELMON-NOR is the first Norwegian study conducted to investigate practices related to telemetry monitoring. All patients assigned to telemetry monitoring were continuously enrolled. Data were collected 24/7 for a period of four to twelve weeks, in 2010, 2015 and 2019. In total, 3,000 patients were included. Both Haukeland University Hospital, Stavanger University Hospital and Oslo University Hospital, Rikshospitalet have contributed to the study.
Arrhythmia incidence, interventions and duration of telemetry monitoring
In total, 33% of monitored patients were diagnosed with an arrhythmia during their hospital stay. More than half of these had to be treated with either medications or other measures, such as cardioversion or pacemaker implantation. The incidence of cardiac arrhythmias were highest in patients with chest pain, syncope or heart failure. Few life-threatening arrhythmias were uncovered during monitoring. More than half of patients admitted due to chest pain are discharged with a diagnosis of myocardial infarction. Almost all patients were undermonitored according to international guidelines.
Patients admitted with a suspicion of cardiovascular disease as cause of the chest pain, must be monitored continuously. If there is a clear suspicion that syncope before admission is due to an arrhythmia, these patients should also be closely monitored. Both of these main findings are commented by the American Heart Association (AHA) in the article Update to Practice Standards for Electrocardiographic Monitoring in Hospital Settings: A Scientific Statement from the American Heart Association (Circulation, 2017). These findings have contributed to patients with a diagnosis of chest pain and syncope being upgraded from Class 2 (should be monitored) to Class 1 (should be monitored by telemetry).
Read the article with the results from our Norwegian study here
Arrhythmia and long-term survival of patients monitored for acute coronary syndrome
In 2009-2010, close to 1,200 patients were included in the TELMON-NOR study. In total, 422 patients were monitored with telemetry due to confirmed acute coronary syndrome. Only 23% of these patients experienced arrhythmias during the hospital stay. Of these, 1.4% were registered as serious events. No difference was found in seven-year survival rate between patients who experienced arrhythmias and those who did not. These results were presented at the American Heart Association Scientific Sessions in 2017.
Read the results from the study
Challenging to change practices
Correct electrode placement and good signal quality are crucial for correct interpretation of arrhythmias and for the implementation of necessary follow-up and treatment. Several studies in TELMON-NOR have revealed that electrode placement is not always optimal, that protective covers to ensure good hygiene are not necessarily used, and that information about the purpose of the monitoring may be deficient. In an intervention study, we tried to change practice. This turned out to be challenging.
Read the results from the intervention study here.
Nurses’ knowledge about the practical use of telemetry
The aims of the study were to determine cardiovascular nurses' knowledge of and adherence to practice standards for cardiac surveillance and whether their knowledge and practice improves over time. A cross sectional study design was applied and data were obtained at the National Congress on Cardiovascular Nursing in 2011 and 2017, in which nurses from 44 and 38 hospitals participated. In total, 185 (68%) of the participants responded to the survey in 2011 and 178 (72%) in 2017. Few participants were aware of international guidelines for telemetry monitoring. Most of them wanted local guidelines. Skin rubbing was often or always performed by 6%, while skin shaving was performed by 94. A protective cover on telemetry units were often or always performed by 65%. Sixty-four percent often or always informed patients of the purpose of the monitoring. Failure to adhere to local and international guidelines may lead to inadequate monitoring, and worsen patient outcomes.
Read the article
Local guidelines for monitoring
Local guidelines for in-hospital telemetry monitoring at Haukeland University Hospital were based on results from the first TELMON-NOR study. These guidelines are currently used at several hospitals in Norway. The guidelines were revised in 2020 based on AHA's revised guidelines for telemetry monitoring from 2017.
Read the article
Read the updated US guidelines from 2017
Call for European guidelines for telemetry monitoring
In 2018, an editorial was published in the European Heart Journal Acute Cardiovascular Care, calling for an initiative from relevant European Society of Cardiology (ESC) bodies to develop European practice standards for in-hospital telemetry monitoring.
Tone M. Norekvål, PhD, RN, Professor, University of Bergen and the Western Norway University of Applied Sciences. Chair of PROCARD research group, Department of Heart Disease, Haukeland University Hospital.
e-mail: tone.merete.norekval@helse-bergen.no
Nina Fålun, MSc, Intensive Care Nurse, Clinical Nurse Researcher, Department of Heart Disease, Haukeland University Hospital, and Senior Lecturer at the Western Norway University of Applied Sciences.
Telephone: +47 55974469
e-mail: nina.falun@helse-bergen.no
Marianne Holm is specialized in intensive care nursing, and is a PhD-candidate at the Western Norway University of Applied Sciences, Bergen. The aim of the PhD project is to investigate whether the monitored population may have changed over the last 10 years, including whether new treatment options may have changed the frequency and severity of the cases of arrhythmia. We will also investigate whether there are patients who should be monitored, but are not, based on current standards - and whether this affect patient outcomes. Sleep deprivation and experiences of delirium have been registered in patients who are monitored with in-hospital telemetry over time. However, knowledge on how patients experience being monitored by in-hospital telemetry is scarce. This will be investigated through in-depth interviews.
PhD student
Marianne Holm, MSc, Intensive Care Nurse, PhD-candidate at the Western Norway University of Applied Sciences, Bergen.
Telephone: +47 905 55 809
Mail: marianne.setrang.holm@hvl.no
Main supervisor
Tone M Norekvål; Professor, University of Bergen and Western Norway University of Applied Sciences. Chair PROCARD research group, Department of Heart Disease, Haukeland University Hospital.
e-mail: tone.merete.norekval@helse-bergen.no
Co-supervisors
Nina Fålun: MSc, Specialized in intensive care nursing, Department of Heart Disease, Haukeland University Hospital and senior lecturer at Western Norway University of Applied Sciences.
Telephone: +47 55974469
e-mail: nina.falun@helse-bergen.no
Bjørn Bendz: MD, Head, Intensive Coronary Care Unit, Department of Cardiology, Oslo University Hospital, PhD, University of Oslo.
Telephone: +47 23 07 00 00
e-mail: bbendz@ous-hf.no
Roy Miodini Nilsen, Biostatistician and professor at the Western Norway University of Applied Sciences.
Telephone: +47 55585648
e-mail: Roy.Miodini.Nilsen@hvl.no